
What is Root Cause Analysis in Medical Billing? Process, Examples & Benefits
If you’re facing continuous denials and want to know the cause behind it, you need to follow a systematic process – that’s known as root cause analysis.
In the U.S. healthcare industry, Continuous claim denials are rarely isolated events. In most cases, they stem from recurring coding errors, documentation gaps, eligibility mismatches, or payer-specific compliance issues. To stop common billing errors, you must identify the root cause and implement strategies to prevent future claim rejections. But conducting RCA can be complicated if not followed via structured steps – so, before doing it, make sure you have a complete understanding of the root cause analysis process in medical billing.
In this guide, you will learn;
- What is a root cause analysis
- Why is RCA important in medical billing
- What’s the purpose behind RCA
- What are the top benefits of root cause analysis
- Step-by-step process of RCA for claim denials
Definition of RCA (Root Cause Analysis)
Root Cause Analysis (RCA) is a systematic, structured process for identifying the underlying causes of problems. By identifying the root cause, you can solve the main issue rather than overlooking the symptoms.
Here are some examples that might help you understand what root cause analysis is in a better way;
Scenario 3: Let’s assume you submit the claims to the insurance company, but they reject the claims. Now, your billing team starts investigating why the claim was rejected, such as a modifier issue or unverified pre-approvals. This way, you’ll identify the root cause and solve the problem for a smooth medical billing process.
What is the Purpose of a Root Cause Analysis
The purpose of a root cause analysis in medical billing is simple and clear: identify the underlying problems, solve them, and ensure they do not recur.
Further, it’s not only about finding the problems — it’s about investigating them in detail, planning a strategic solution, and implementing it promptly. In the denial management context, the purpose of root cause analysis is to determine the root cause by examining denial codes, resolving the issues, and then building the best strategies to prevent recurrence.
How to Perform Root Cause Analysis for Claim Denials
To conduct a root cause analysis for claim denials, you should follow a thorough set of steps that will help you achieve what you’ve lost – your practice’s revenue.
Here’s the root cause analysis procedure you should follow;
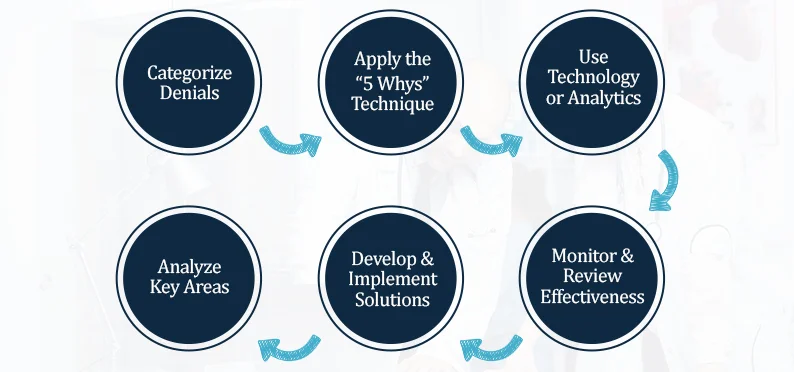
Categorize Denials
The standard rule for beginning root cause analysis is to identify the problem first. What happened? Once you know what the issue is, you will be able to find the reason then.
To identify denials in medical billing, start by categorizing them based on all available data. Once you have recorded data such as EOB/ERA explanations, CARA/RARC codes, and the medical claims you submitted, then you’ll be able to identify which type of denials occurred.
Do you want to learn more about denial codes and how to handle them? Read the full guide now!
Apply the “5 Whys” Technique
In the RCA process, another common method is using the 5 Whys technique. It’s the most effective approach, yet it helps practices identify root causes efficiently and easily.
What you should do is to ask 5 WHY questions – such as Why does the payer reject the claim? And you got the first answer, the CPT code is incorrect. Then again, think about why it is. Likewise, ask 5 times why to dig deeper until you get the main source of the problem (denial).
Use Technology or Analytics
By using medical billing software, checking KPIs, and analytics, you’ll be able to track denials easily, as it notifies you about the trend of denials and why they occur.
Analyze Key Areas
After categorizing the denials, using the 5 Whys technique and RCM software analytics, you’ll be able to identify the key factors driving denials. Ensure you record every factor you track, including the coding error rate (5%), pre-authorization issues (7%), and missing modifiers (approximately 4%).
Once you identify the key areas that lead to denials, you’ll be able to pinpoint the root cause, such as a medical coding executive being a newbie or using outdated code, pre-authorization checks expiring, or being forgotten by the front-desk staff to verify before or during a patient visit. Hence, it all helps you create a plan to control these mistakes from happening again.
Develop & Implement Solutions
Once you have identified the root cause of denials, develop a strategic plan to address the issues. The action plan must involve the solutions or steps you should take to address the problems. For example, train staff, update software, or analyze billing workflows, then implement these solutions to recurring root causes.
Monitor & Review Effectiveness
Developing and implementing an action plan isn’t enough – you need to monitor to verify whether it’s working continuously. Using medical billing software can help you assess the plan’s effectiveness and ensure denials don’t recur due to the same reasons.
What are the Top Benefits of Root Cause Analysis
There are various benefits of the root cause problem-solving process. Let’s uncover the top benefits of error-cause identification (RCA) in healthcare billing.

Improved Compliance & Audit Safety
The most beneficial part of conducting quality issue analysis (RCA) is that you can improve compliance and safe, aggressive audits from insurance payers. How’s that possible? It’s all because root cause analysis helps you find the major issue behind the denials, such as a medical claim that didn’t fully follow the payer policy and HIPAA rules. In this way, practices can develop a strategic plan and ensure that the billing team follows patient safety rules and protects patient data in accordance with HIPAA, thereby avoiding future audits or high penalties.
Reduced Denials & Increased Revenue
Root cause problem-solving minimizes common medical billing errors, such as incorrect patient demographics and unverified credentials before claim submission, thereby supporting a clean claim rate and a smooth reimbursement cycle.
Improved Efficiency & Reduced Costs
By identifying issues, billing professionals don’t need to repeatedly work on the same denied claims, improving overall billing efficiency and reducing operational costs.
Make Informed Decisions
By performing the RCA process, you can make better decisions on how to improve revenue cycle management, administrative, and clinical operations efficiency, offering the best possible care while protecting money.
Better Patient Engagement
Conducting RCA gradually helps you identify gaps and compliance issues, and manage billing tasks effectively to control claim rejections. By doing this, practices can improve RCM operations, reduce workload, and help providers focus more on what matters most – patient care.
How eClaim Conducts Root Cause Analysis to Identify Denials
Managing denials isn’t as easy as submitting claims – it requires expertise, and professionals who know the difference between soft and hard denials to create a strong appeal that helps recover lost revenue.
To identify denials, the first step you should take is to conduct root cause analysis – that’s exactly what eClaim Solution exactly does. Our RCA experts have years of experience and stay up to date on current healthcare policies to reduce denials effectively.
Here’s how our experts perform root cause analysis;
- Begins by checking what denial code appears and what the error is.
- After identifying the symptoms, our RCA professionals check how many claims are affected.
- Gather the required data, such as medical necessity documents, EOB/ERA explanations, and physicians’ clinical notes.
- Identify the cause, where the problem occurs, during the patient appointment, medical coding, or claim submission.
- Use the “5 Whys” technique to identify the most accurate root cause and determine whether it has been solved; if not, does it recur in denials?
- Utilizing advanced tools and RCA methods, such as a fishbone diagram, to map out the failure points.
- Generate an action plan to solve the identified problems and assign the task to implement it.
- Track, monitor, and analyze whether the strategies worked.
Frequently Asked Questions
Root cause analysis (RCA) is a systematic and structured process that helps identify the underlying issue of the problem, or we can say what’s the core reason behind it.
To conduct a root cause analysis, one should follow simple steps: identify the problem, collect data, apply techniques and approaches, determine the root cause, plan how to solve it, implement the solutions, and monitor until the problem is resolved.
The most common RCA mistakes are stopping on symptoms, shifting the blame to humans, even if it’s technical, relying on assumptions instead of collecting evidences/facts, and forgetting to monitor the recommendations, whether they are implemented or not.
Book a Consultation
Categories
- ╰┈➤ Medical Billing
- ╰┈➤ Specialty Billing
- ╰┈➤ Credentialing
- ╰┈➤ Medical Coding
Table of Content
- Definition of RCA (Root Cause Analysis)
- How to Perform Root Cause Analysis for Claim Denials
- What are the Top Benefits of Root Cause Analysis
- How eClaim Conducts Root Cause Analysis to Identify Denials
- FAQs
Comprehensive Healthcare Management Services
